Disease Overview
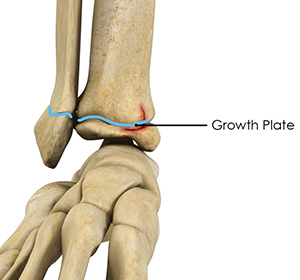
Growth plates, also called the epiphyseal plate or physis, are the areas of growing cartilaginous tissue found at the ends of the long bones in children. These growth plates determine the length and shape of the mature bone. The growth plates are more susceptible to damage from trauma because they are not as hard as bones.
Growth plate injuries commonly occur in growing children and teenagers. In children, severe injury to the joint may result in a growth plate fracture rather than a ligament injury. Any injury that can cause a sprain in an adult can cause a growth plate fracture in a child.
Growth plate fractures are more common in boys than girls because the plates develop into mature bone faster in girls. Growth plate fractures commonly occur at the wrist, long bones of the forearm (radius) and fingers (phalanges), legs ( tibia and fibula), foot, ankle or hip during sports activities such as football, basketball and gymnastics.
Types of growth plate fractures
Growth plate fractures can be classified into five categories based on the type of damage caused.
- Type I – Fracture through the growth plate: The epiphysis is separated from the metaphysis with the growth plate remaining attached to the epiphysis. The epiphysis is the rounded end of the long bones below the growth plate and the metaphysis is the wider part at the end of the long bones above the growth plate.
- Type II – Fracture through the growth plate and metaphysis: This type is the most common type of growth plate fracture. The growth plate and metaphysis are fractured without involving the epiphysis.
- Type III – Fracture through the growth plate and epiphysis: In this type of injury, the fracture runs through the epiphysis and separates the epiphysis and growth plate from the metaphysis. It usually occurs in the tibia, one of the long bones of the lower leg.
- Type IV – Fracture through growth plate, metaphysis, and epiphysis: Type IV is when the fracture goes through the epiphysis and growth plate, and into the metaphysis. This type often occurs in the upper arm near the elbow joint.
- Type V – Compression fracture through growth plate: This type of fracture is a rare condition where the end of the bone gets crushed and the growth plate is compressed. It can occur at the knee or ankle joint.
Causes
Growth plate injuries are caused by accidental falls or blows to the limbs during sports activities such as gymnastics, baseball, or running. They may also result from overuse of tendons and certain bone disorders such as infection that can affect the normal growth and development of the bone. The other possible causes which can lead to growth plate injuries are:
- Child abuse or neglect – Growth plate fractures are one of the most common fractures that occur in abused or neglected children.
- Exposure to intense cold (frostbite) – Extremely cold climatic conditions can cause damage to the growth plates resulting in short fingers and destruction of the joint cartilage.
- Chemotherapy and medications – Chemotherapy to treat cancer in children and continuous use of steroids for arthritis may affect bone growth.
- Nervous system disorders – Children with disorders of the nerves may have sensory deficits and muscular imbalances that can cause them to lose their balance and fall.
- Genetic disorders – Gene mutations may result in poorly formed or malfunctioning growth plates which are vulnerable to fracture.
- Metabolic diseases – Diseases such as kidney failure and hormonal disturbances affect the proper functioning of the growth plates and increase susceptibility to fractures.
Signs and symptoms
Signs and symptoms of a growth plate injury include:
- Inability to move or put pressure on the injured extremity
- Severe pain or discomfort that prevents the use of an arm or leg
- Inability to continue playing after a sudden injury because of pain
- Persistent pain from a previous injury
- Malformation of the legs or arms as the joint area near the end of the fractured bone may swell.
In children, fractures heal faster. If a growth plate fracture is left untreated it may heal improperly causing the bone to become shorter and abnormally shaped.
Diagnosis
Your doctor will evaluate the condition by asking you about the injury and performing a physical examination of the child.
X-rays may be taken to determine the type of fracture. Since the growth plates have not hardened and may not be visible, X-rays of the injured as well as the normal limb are often taken to look for differences in order to help determine the place of injury.
Other diagnostic tests your doctor may recommend include computed tomography (CT) scan or magnetic resonance imaging (MRI). These tests are helpful in detecting the type and extent of the injury as it allows the doctor to see the growth plate and soft tissues.
Treatment
The treatment for growth plate injuries depends upon the type of fracture involved. In all cases, the treatment should begin as early as possible and include the following:
- Immobilization: The injured limb is covered with a cast or a splint may be given to wear. The child will be advised to limit activities and avoid putting pressure on the injured limb.
- Manipulation or surgery: If the fracture is displaced and the ends of the broken bones do not meet in the proper position, then your doctor will unite the bone ends into the correct position either manually (manipulation) or surgically. Sometimes, a screw or wire may be used to hold the growth plate in place. The bone is then immobilized with a cast to promote healing. The cast is removed once healing is complete
- Physical therapy: Exercises such as strengthening and range-of-motion exercises should be started only after the fracture has healed. These are done to strengthen the muscles of the injured area and improve the movement of the joint. A physical therapist will design an appropriate exercise schedule for your child.
- Long-term follow-up: Periodic evaluations are needed to monitor the child’s growth. Evaluation includes X-rays of matching limbs at intervals of 3 to 6 months for at least 2 years.
Risks and complications
Most growth plate fractures heal without any long-term problems. Rarely, the bone may stop growing and become shorter than the other limb.







